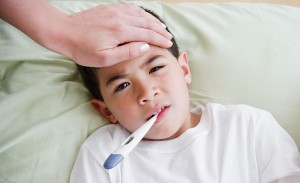
Cold weather is traditionally accompanied by a morbidity season lift: fever, cough, runny nose, headache, malaise and, as a result, antibiotics. What do you need to know about them? Canadian Family Pharmacy Corp have selected the most popular questions about them:
1. What is the action of antibiotics?
Antibiotics classification is based on the mechanism of their action:
- Bactericidal antibiotics;
- bacteriostatic antibiotics.
Antibacterial ones kills germs, while bacteriostatic ones break the cycle their development, preventing further proliferation of the microbe.
2. In what cases it is necessary to use antibiotics and when are they useless?
You can’t go without antibacterial drugs in cases of bacterial infections.
There are two main groups of infections:
- Viral infections;
- bacterial infections.
There are some other options – fungal, protozoal infections and so on, but that’s a topic for another conversation. In cases of viral infections antibiotics are not prescribed, but in case of bacterial infections – they are required. For example, influenza is a viral infection, and antibiotics for a flu are not prescribed. And acute tonsillitis (angina) is a bacterial infection, and the prescription of an antibiotic is necessary. Antibiotics are also used in COPD treatment.
It should be noted that the majority of infections are virus ones. But despite this fact, excessive use of antibiotics makes about 60%, in the world – about 40%, according to Canadian Family Pharmacy statistics.
3. How to distinguish a virus from a bacterium?
It is the task of the physician. Antibiotics should be used only in case there is a clearly proven bacterial infection, or clinically, for example, the doctor sees purulent otitis, acute tonsillitis – then an antibiotic is taken immediately and unconditionally, or there is laboratory confirmation: changes in the general analysis of blood, certain figures in the biochemical analysis blood, microbe seeding of the bacterial outbreak, as well as the epidemiological evidence.
4. What is a danger of antibiotics overdose?
 Not only uncontrollable intake of antibiotics is dangerous, but also the wrong antibiotics. An uncontrolled reception is an independent intake of antibacterial drugs without consulting a doctor. A wrong intake relates to a wrong dosage, dosing frequency and duration of the course.
Not only uncontrollable intake of antibiotics is dangerous, but also the wrong antibiotics. An uncontrolled reception is an independent intake of antibacterial drugs without consulting a doctor. A wrong intake relates to a wrong dosage, dosing frequency and duration of the course.
An uncontrolled intake and wrong methods are fraught with the same consequences: generation of resistant forms. Over time the bacteria adapt to the environment and to the used antibiotics. As a result of improper use of antibiotics, the bacteria are not completely destroyed and develop certain enzymes which destroy the antibiotic over time.
It is important to understand that if the dose is less than required, it will not help. If the dosing frequency is less than necessary, it will not help. If the duration of the course is less than required, it will not help. If you are prescribed to take antibiotics for seven days, then take it seven days, not three and not six. Antibiotics should finally fulfill their role, otherwise the surviving bacteria will gradually form mechanisms of resistance, and one day antibiotics will cease to act properly. Overdose may intensify antibiotics side-effects.
What is the result? Today scientists discuss a very serious matter that “working” antibiotics will disappear in the next couple of decades.
5. People say that the minimum course of antibiotic therapy is five days, is it so?
We can not give a definite answer to this question, because there are different groups of antibacterial drugs. There are drugs that are administered once a month, there are drugs that one need to be take three, fourteen, twenty-one days. Antibiotics are individual and prescribed by a doctor.
6. Do antibacterial drugs influence the gastrointestinal tract? Is it necessary to deal with it?
 Such fears appeared when semisynthetic penicillins in a tablet form have gained a wide spread, people started to take them in cases of any diseases. These drugs actually caused:
Such fears appeared when semisynthetic penicillins in a tablet form have gained a wide spread, people started to take them in cases of any diseases. These drugs actually caused:
- Disturbance of the intestinal micro flora;
- disbiotic processes;
- mycosis (fungal).
Today children over the age of 1 year, as a rule, have no distinct dysbiotic phenomena in the case of uncomplicated bacterial infection (on the condition of not very long treatment course (no more than 10 days).
It is important to know that only lactobacilli survive with antibiotics, so if the antibiotic therapy developed symptoms of dysbiosis, you will have to complete the course of antibiotics therapy first, and then start a course of complex biologics.
In some situations, such as when taking macrolide antibiotics, the presence of diarrhea generally does not speak about the presence of dysbiosis, as a chemical formula of macrolide antibiotics acts as a laxative. In such situations disbiotic symptoms disappear at the end of the treatment with antibiotics.
7. Do antibiotics have symptomatic action?
Antibiotics have no effect on the symptoms. They do only one thing: kill the bacteria (if there is any).
Antibacterial drugs:
- Do not reduce the temperature;
- do not affect the cough;
- do not reduce toxicity;
- do not eliminate the headache.
If bacteria is not present, antibiotics will not help.
8. Can I drink antibiotics to prevent disease?
Antibiotics has no prophylactic effect. If bronchitis or pneumonia occur as a complication of influenza, and you started to take an antibiotic “just in case” before this complication, the process will still develop, but the germ that caused it, will be insensitive to this antibiotic.
Remember: only a doctor can prescribe antibiotics! Besides, it’s necessary to purchase antibiotics only from tried pharmacies. Canadian Family Pharmacy is an example of such pharmacy which always takes care of its clients. Here you may buy antibiotics online on affordable conditions: Amoxicillin, Zithromax, Bactrim, Cephalexin, Stromectol! Be healthy!